In today’s fast-paced world, technology has become an integral part of healthcare. From Electronic Health Records (EHR) systems to telemedicine apps, healthcare software is transforming the way care is delivered. Yet, building software for the healthcare industry isn’t just about writing code; it involves understanding regulatory requirements, ensuring data security, and prioritizing patient outcomes. In this guide, we’ll explore the ins and outs of healthcare software product development, focusing on the stages, challenges, and best practices involved.
What is Healthcare Software Product Development?
Healthcare software product development refers to the process of creating software specifically designed to meet the needs of healthcare providers, patients, and other stakeholders in the healthcare ecosystem. This includes building applications that streamline operations, improve patient outcomes, and ensure compliance with regulatory standards.
👉 Curious About Development Costs? Use our Free App Cost Calculator to estimate your healthcare product budget in minutes—no sign-up needed!
Calculate NowTypes of Healthcare Software Products
Electronic Health Records (EHR) Systems – Digitally store and manage patient health information for clinical workflows.
Electronic Medical Records (EMR) Systems – Clinic-specific systems focused on the digital version of paper charts.
Telemedicine Software – Enables remote consultations between patients and healthcare providers.
ePrescription Software – Allows providers to send prescriptions electronically to pharmacies.
Hospital Management Systems (HMS) – Manage hospital operations including patient intake, billing, and administration.
Medical Billing Software – Automates claim generation, insurance verification, and revenue cycle management.
Patient Portals – Empower patients with access to their health data, appointments, and secure communication.
Remote Patient Monitoring (RPM) Software – Tracks patient vitals and symptoms using connected health devices.
Clinical Decision Support Systems (CDSS) – Assist clinicians in making data-driven decisions through alerts and recommendations.
Laboratory Information Systems (LIS) – Manage lab workflows, sample tracking, and diagnostic reporting.
Radiology Information Systems (RIS) – Organize and manage medical imaging data and workflows.
Picture Archiving and Communication Systems (PACS) – Store, retrieve, and share digital medical images.
Medical Research & Clinical Trial Software – Support clinical studies with protocol tracking, EDC, and data analysis.
Mental Health Apps – Provide digital therapy, mood tracking, and self-help for mental wellness.
Fitness & Wellness Apps – Help users monitor physical activity, sleep, nutrition, and fitness goals.
Chronic Care Management Software – Enables continuous monitoring and care plans for chronic condition patients.
Pharmacy Management Software – Streamlines drug inventory, prescriptions, and compliance tracking.
Healthcare CRM Systems – Centralize patient interactions, follow-ups, and outreach automation.
Medical Inventory Management Software – Tracks and automates stock, supplies, and usage in healthcare settings.
Home Healthcare Software – Manages caregivers, schedules, and services for in-home patient care.
Healthcare Analytics Platforms – Use data visualization and predictive analytics to improve outcomes and reduce costs.
Health Insurance Software – Supports claims processing, policy management, and member engagement.
Medical Practice Management Software – Integrates scheduling, billing, documentation, and patient records.
Occupational Health Software – Designed for workplace health tracking, compliance, and employee health records.
Rehabilitation Software – Guides therapy workflows, progress tracking, and patient recovery programs.
Build Software That Meets Regulatory Compliances like HIPAA
Connect with expertsWhy Healthcare Software Product Development is Essential
The demand for healthcare software has skyrocketed, and for good reason. The healthcare landscape is constantly evolving, and healthcare providers need modern solutions to keep up with these changes.
Meeting the Needs of Modern Healthcare Providers
Doctors, nurses, and administrators rely heavily on software to manage patient data, streamline workflows, and enhance communication between departments.
Enhancing Patient Care
Healthcare software allows for real-time access to critical patient information, resulting in quicker diagnoses and better care coordination.
Addressing Regulatory and Compliance Demands
Healthcare is one of the most regulated industries. Developing compliant software ensures healthcare organizations meet standards such as HIPAA, ensuring patient privacy and data security.
Key Features of Effective Healthcare Software
When developing healthcare software, there are essential features that should always be included:
User-Friendly Interface
Healthcare professionals are busy, and they need software that is intuitive and easy to use, without a steep learning curve.
Data Security and HIPAA Compliance
Ensuring the security of sensitive patient information is paramount. All healthcare software must comply with HIPAA regulations, safeguarding patient data.
Interoperability and Data Integration
Healthcare software should easily integrate with existing systems and facilitate seamless data exchange between platforms.
Real-Time Analytics and Reporting
Healthcare providers need access to real-time data and analytics to make informed decisions, enhance care, and monitor outcomes.
Understanding the Healthcare Software Development Lifecycle
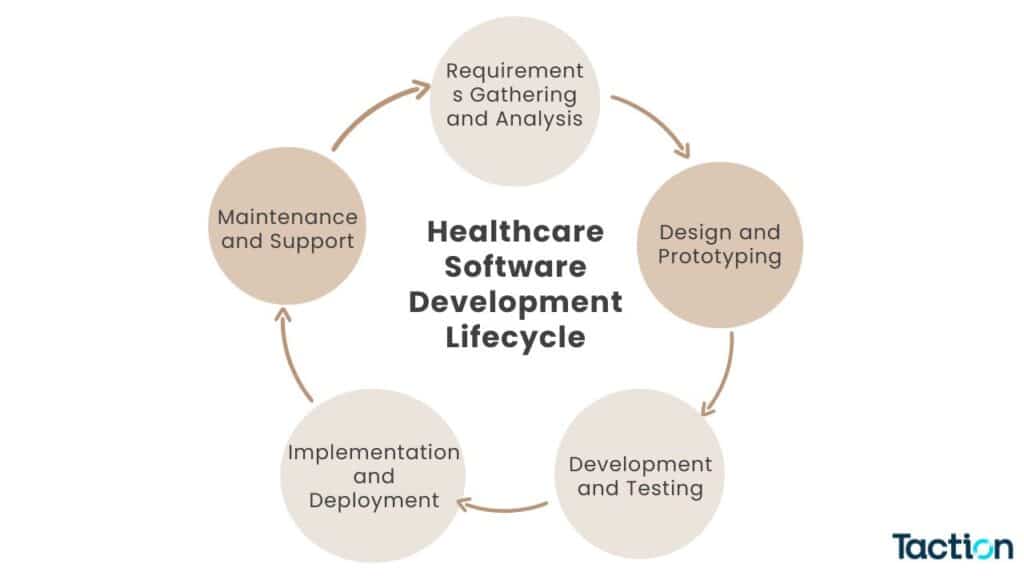
Healthcare software development follows a series of structured steps, each critical to the final product’s success.
Requirements Gathering and Analysis
The first step involves identifying the needs of stakeholders, including healthcare providers, patients, and administrators.
Design and Prototyping
Once requirements are gathered, developers create prototypes to visualize the software’s functionality and user experience.
Development and Testing
During the development phase, the actual coding takes place, followed by rigorous testing to ensure the software is bug-free and performs as expected.
Implementation and Deployment
After testing, the software is deployed in the healthcare environment. This stage often requires training for end-users, such as doctors and nurses.
Maintenance and Support
Post-launch support is crucial for ensuring long-term software success, including regular updates, bug fixes, and performance improvements.
Regulatory Considerations in Healthcare Software Development
Developing healthcare software isn’t just about meeting user needs—it’s also about adhering to strict regulatory standards.
HIPAA Compliance
HIPAA (Health Insurance Portability and Accountability Act) outlines the legal requirements for protecting patient data in the United States. Ensuring HIPAA compliance is a non-negotiable aspect of healthcare software development.
FDA Approval for Medical Devices and Software
Certain healthcare software, especially those classified as medical devices, may require FDA approval to ensure they meet safety and efficacy standards.
GDPR Compliance
If your healthcare software will serve European users, you must ensure compliance with the General Data Protection Regulation (GDPR), which governs data privacy and security.
Challenges in Healthcare Product Development & How to Overcome Them
Bringing a healthcare software product to life involves far more than writing code. It demands architectural foresight, compliance rigor, and seamless system interoperability. Let’s break down the most common challenges and how to address them effectively.
1. Embedding Compliance into the Architecture
Healthcare applications must comply with standards like HIPAA, GDPR, HITECH, and PIPEDA, depending on the geography. This involves architecting the solution to support:
Role-based access control (RBAC)
End-to-end encryption (AES-256, TLS 1.3)
Audit logging
Data retention policies
Security must be baked into the backend via token-based authentication (e.g., OAuth 2.0), secure API gateways, and database-level encryption—not just handled at the surface layer.
2. Achieving Seamless Interoperability
Interfacing with existing EHRs, HIEs, and clinical systems is a persistent hurdle. Integration requires:
Support for FHIR, HL7 v2/v3, DICOM, and CCDA
Custom interface engines or use of platforms like Mirth Connect
Data mapping, cleansing, and semantic normalization layers
Without this, data exchange remains fragmented and unscalable. A dedicated integration layer using microservices or middleware helps unify healthcare data flow.
3. Ensuring Scalable and Performant Architecture
As healthcare products scale, latency and availability become critical. Core solutions include:
Event-driven architecture using tools like Kafka or RabbitMQ
Scalable containerization via Docker + Kubernetes
Distributed databases (e.g., MongoDB, PostgreSQL with partitioning)
Implementing auto-scaling, background job queues, and performance monitoring (Prometheus, ELK stack) ensures the app handles peak loads without compromising speed or security.
4. Balancing Clinical Usability with Technical Complexity
Medical professionals require intuitive workflows, not technical hurdles. However, the complexity of features like charting, e-prescriptions, and decision support systems often creates friction.
Solutions include:
Clinical co-design sessions during UX prototyping
Figma-based wireframes validated by end users
A/B tested onboarding experiences
This ensures that even technically robust systems remain accessible to non-technical users in real clinical environments.
5. Enabling Agile and DevSecOps Practices
Frequent updates, quick patches, and regulatory audits demand an agile pipeline with security-first development.
Implement:
CI/CD pipelines using Jenkins, GitHub Actions, or GitLab CI
Infrastructure as Code (IaC) via Terraform or Ansible
Static code analysis and vulnerability scanning in every build
These practices reduce technical debt while ensuring compliance and speed.
Compliance Standards: HIPAA, HL7, and FHIR Explained Simply
Compliance isn’t just a checkbox—it’s the foundation of trust, security, and interoperability in any healthcare product. Here’s a simplified breakdown of the most essential standards every healthcare software team must understand and implement.
1. HIPAA: Protecting Patient Privacy in the U.S.
The Health Insurance Portability and Accountability Act (HIPAA) is the gold standard for safeguarding protected health information (PHI) in the United States. It mandates that healthcare applications must:
Encrypt data at rest and in transit
Implement access controls and user authentication
Maintain audit logs and breach reporting
Sign Business Associate Agreements (BAAs)
Failure to comply can result in fines up to $1.5 million per year. Solutions often involve secure cloud infrastructure (e.g., AWS HIPAA-eligible services) and robust user permission models.
2. HL7: The Legacy Language of Health Data
HL7 (Health Level Seven) is a set of international standards for the transfer of clinical and administrative data. HL7 v2, the most widely used, facilitates system-to-system messaging (e.g., lab results, admissions, discharges).
Why it matters:
Powers communication between EHRs, LIS, RIS, and other hospital systems
Requires use of HL7 message segments (e.g., MSH, PID, OBX)
Often implemented using tools like Mirth Connect for mapping and transformation
Though older, HL7 is still essential for working with legacy health IT infrastructure.
3. FHIR: The Modern API-Based Interoperability Standard
FHIR (Fast Healthcare Interoperability Resources) is the future of healthcare data exchange. It uses RESTful APIs and modern web standards like JSON and XML to make data portable and accessible.
Why developers love it:
Easy to implement with standard HTTP methods (GET, POST, PUT, DELETE)
Resource-based approach (e.g., Patient, Observation, Encounter)
Built-in versioning, extensibility, and security models
FHIR makes it easier to build mobile apps, patient portals, and clinical decision support tools while ensuring interoperability across systems.
Key Takeaway
To build a compliant and future-ready healthcare product, it’s not enough to just know HIPAA, HL7, and FHIR—you need to embed them directly into your software architecture and workflows.
Best Practices for Healthcare Software Development
To ensure the success of your healthcare software, consider the following best practices:
Engaging with End-Users for Feedback
Consulting with doctors, nurses, and patients during development ensures that the software meets their needs and is user-friendly.
Prioritizing Data Security from the Start
Data security should be a primary focus from the beginning, with robust encryption, secure access controls, and regular security testing.
Focusing on Scalability
Your software should be built to scale, accommodating future growth and technological advancements.
Iterative Development and Regular Updates
An iterative development approach, such as Agile, allows for continuous improvement and adaptation based on user feedback and changing needs.
Top Tech Stacks in 2025 for Healthcare Product Engineering
Choosing the right technology stack is critical for building scalable, secure, and regulation-compliant healthcare products. In 2024, the healthcare industry is leaning towards modern, cloud-native, and API-first architectures that enable rapid development, seamless integrations, and data-driven insights.
1. Frontend Technologies
React.js – Preferred for building fast, component-based web interfaces with reusable UI elements and virtual DOM performance.
Next.js – Ideal for server-side rendering (SSR) and improved SEO in patient-facing apps.
Flutter / React Native – For cross-platform mobile app development with near-native performance and a single codebase.
2. Backend Technologies
Node.js – High concurrency and event-driven architecture make it suitable for real-time updates and scalable APIs.
Python (Django/FastAPI) – Popular for AI/ML-based healthcare features and secure RESTful API development.
Java (Spring Boot) – Often used in enterprise-grade applications due to its strong security and multithreading capabilities.
3. Databases
PostgreSQL – A go-to RDBMS with ACID compliance and support for JSONB, suitable for structured clinical data.
MongoDB – Flexible document storage for unstructured data like logs, patient forms, or symptom reports.
Redis – Used for caching to ensure faster data retrieval in real-time dashboards and patient monitoring apps.
4. Cloud & DevOps
AWS / Google Cloud / Azure – HIPAA-compliant cloud services for hosting, file storage, and managed Kubernetes.
Docker & Kubernetes – Containerized deployments and orchestration for modular scaling and infrastructure automation.
CI/CD with GitHub Actions / GitLab CI – For faster release cycles and automated compliance checks.
5. Interoperability & Integration Standards
- FHIR (Fast Healthcare Interoperability Resources) – RESTful APIs for seamless EHR/EMR communication.
- HL7 v2/v3 – Still critical for legacy system compatibility in hospitals and labs.
- Mirth Connect – A powerful integration engine for routing and transforming clinical data across systems.
6. Security Frameworks
OAuth 2.0 / OpenID Connect – For secure, token-based authentication.
AES-256 & TLS 1.3 – For encrypting PHI in transit and at rest.
Snyk / SonarQube – Integrated into pipelines for proactive vulnerability detection.
Summary:
In 2025, healthcare product development requires tech stacks that are not just cutting-edge—but also scalable, compliant, and integration-ready. The right stack isn’t just about performance; it’s about building trust in every transaction, API call, and patient interaction.
Agile Methodology in Healthcare Software Development
The Agile methodology is becoming increasingly popular in healthcare software development. It offers:
- Flexibility: Agile allows for changes to be made during the development process, ensuring the product meets evolving needs.
- Faster Delivery: With sprints and real-time feedback, development progresses quickly.
- Collaboration: Developers, healthcare professionals, and other stakeholders work together throughout the process.
Data Security and Privacy in Healthcare Software Development
Encryption Techniques
All sensitive data should be encrypted to protect against unauthorized access and breaches.
Multi-Factor Authentication (MFA)
MFA adds an additional layer of security by requiring users to verify their identity through multiple methods.
Secure Data Transmission
Ensure secure data transmission using protocols like HTTPS and encryption algorithms.
Interoperability in Healthcare Software
Importance of Interoperability
Interoperability ensures that healthcare providers can access and exchange patient data seamlessly across different systems.
Common Standards
Standards like HL7 and FHIR are widely used to promote data exchange and integration between healthcare systems.
Innovative Trends in Healthcare Software Development
The healthcare industry is always evolving, with several exciting trends on the horizon:
AI and Machine Learning
AI and ML are being used to improve diagnostics, personalize treatment plans, and analyze massive datasets for predictive analytics.
Virtual Reality (VR) in Healthcare
VR is increasingly being used for everything from surgical training to pain management for patients.
Blockchain for Healthcare Data Management
Blockchain offers a decentralized and secure way to store and manage healthcare records, improving data security and transparency.
Case Example: How a Custom Health App Scaled from MVP to 1M Users
Scaling a healthcare application from an MVP to a million active users requires strategic engineering, compliance-first development, and user-centered design. Here’s a breakdown based on a real-world pattern we often see in successful healthcare products.
Phase 1: MVP Launch with Core Clinical Features
The MVP was designed to solve a narrow clinical problem—streamlining symptom tracking and virtual consultations. Built using a React Native frontend, Node.js backend, and Firebase for real-time data, it launched in just 12 weeks with:
HIPAA-compliant authentication (JWT + OAuth 2.0)
Basic EHR integration using FHIR APIs
Real-time symptom logs with push notifications
Feedback loop from early clinicians and patient users
Phase 2: Modular Feature Expansion and Interoperability
Once initial traction was gained (~10K users), we introduced:
HL7 and DICOM support to integrate lab reports and imaging
A microservices architecture using Docker + Kubernetes
Secure messaging module with AES-256 encryption
Role-based access control for providers and patients
This allowed the app to plug into multiple hospital networks without rewriting core logic.
Phase 3: Scaling Infrastructure and Performance
With user base expanding rapidly, we shifted to a multi-region AWS setup, added Redis caching, and implemented horizontal scaling through load balancers and autoscaling groups.
Other key upgrades included:
CI/CD pipelines with GitHub Actions + SonarQube
Logging and monitoring using Prometheus + Grafana
Daily backups and disaster recovery automation
The platform comfortably handled over 50K concurrent users.
Phase 4: Patient Retention and Intelligence Layer
Retention was driven by:
AI-powered recommendations for follow-ups and medication adherence
Gamification (badges for health goals, streaks)
Integration with Apple HealthKit and Google Fit for wearable sync
Today, the app supports over 1 million active users, 10+ healthcare systems, and continues to evolve with advanced features like telehealth, clinical decision support, and population health dashboards.
Build One Medical App with Multiple Opportunities
• Personalized News Feed for Doctors
• Remote Patient Monitoring
• Communication Platform with HIPAA-Compliant
Connect with experts
Conclusion
Healthcare software product development is at the core of modernizing the healthcare industry. From streamlining administrative tasks to improving patient care, the right software can transform healthcare delivery. By following best practices, addressing challenges, and embracing innovation, healthcare providers can build software that meets the needs of today’s fast-paced, ever-evolving healthcare landscape.
FAQs
The cost can vary, typically ranging from $100,000 to millions, depending on the complexity and scope of the project.
The timeline can vary but generally ranges from 6 months to 2 years, depending on the size and complexity.
HIPAA, FDA approval, and GDPR are some of the major compliance requirements for healthcare software.
Data security is ensured through encryption, multi-factor authentication, secure data transmission, and regular security audits.
Custom healthcare software offers tailored solutions, better integration with existing systems, improved user experience, and enhanced security.
The cost can vary, typically ranging from $100,000 to millions, depending on the complexity and scope of the project.
The timeline can vary but generally ranges from 6 months to 2 years, depending on the size and complexity.
HIPAA, FDA approval, and GDPR are some of the major compliance requirements for healthcare software.
Data security is ensured through encryption, multi-factor authentication, secure data transmission, and regular security audits.
Custom healthcare software offers tailored solutions, better integration with existing systems, improved user experience, and enhanced security.




